
Family Reach Blog
Blog Posts


Where Does Your Money Go When You Donate to Family Reach?

Interview with Catharine Arnston CEO of energybits inc in kind sponsor

The Early Roots of Family Reach: Remembering Kristine Morello-Wiatrak

Partnership Spotlight: Anthony Rizzo Family Foundation
Celebrating Maribeths life merrigan family joined community

Family Endures Financial Struggles After Dad Faces Another Cancer Relapse

12 Ways to Save Money During Cancer Treatment

Remembering Pat Kelly

How to Save Money on Food During Cancer Treatment

There’s More to the Story: Marc Benioff

12 Holiday Savings Tips for Families Facing Cancer

7 Quick Tips for Managing Your Finances During Cancer Treatment

Financial Coaching: Top 10 Questions Answered

In Conversation: Chef Ming Tsai On 10 Years of Supporting Family Reach

How Do Social Determinants of Health Affect Cancer Patients?

In Conversation: AbbVie Executive and Family Reach Board Member Melissa Walsh On Career and Community

Turning Loss Into Impact: Nicole Ackerman Shares What Sparked Her Career in Cancer Patient Advocacy

Cancer Survivor and ‘The Patient Story’ Founder Shares the Power of Connection and Community
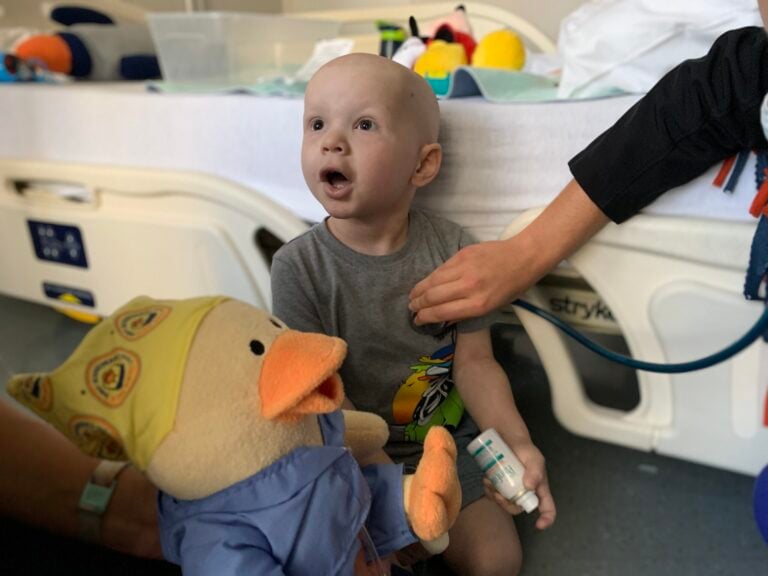
5 Things We Wish We Knew: Parents Share their Tips about Childhood Cancer

There’s More to the Story: Chef Ming Tsai

When Your Child Has Cancer: Letters of Wisdom from Cancer Dads

Cancer Patients Who “Don’t Look Sick” Break Down This Common Misconception

Letters from Cancer Caregivers: How to Support Yourself and Your Loved One

The St. Jude’s Controversy: A Look at Why Family Reach Welcomed the Spotlight on the Financial Reality of Cancer

Letters from Moms with Cancer: Advice for When You’re ‘Mom’ and ‘Patient’

Partnership with Hilton Provides Cancer Patients with a Home Away from Home

5 Questions to Ask Your Hospital Social Worker When Facing a Cancer Diagnosis

6 Free Financial Resources for Cancer Patients and Caregivers

Healing at Home: Overcoming Housing Insecurity for Families Facing Cancer

6 Reasons to Give Monthly to Nonprofit Organizations


